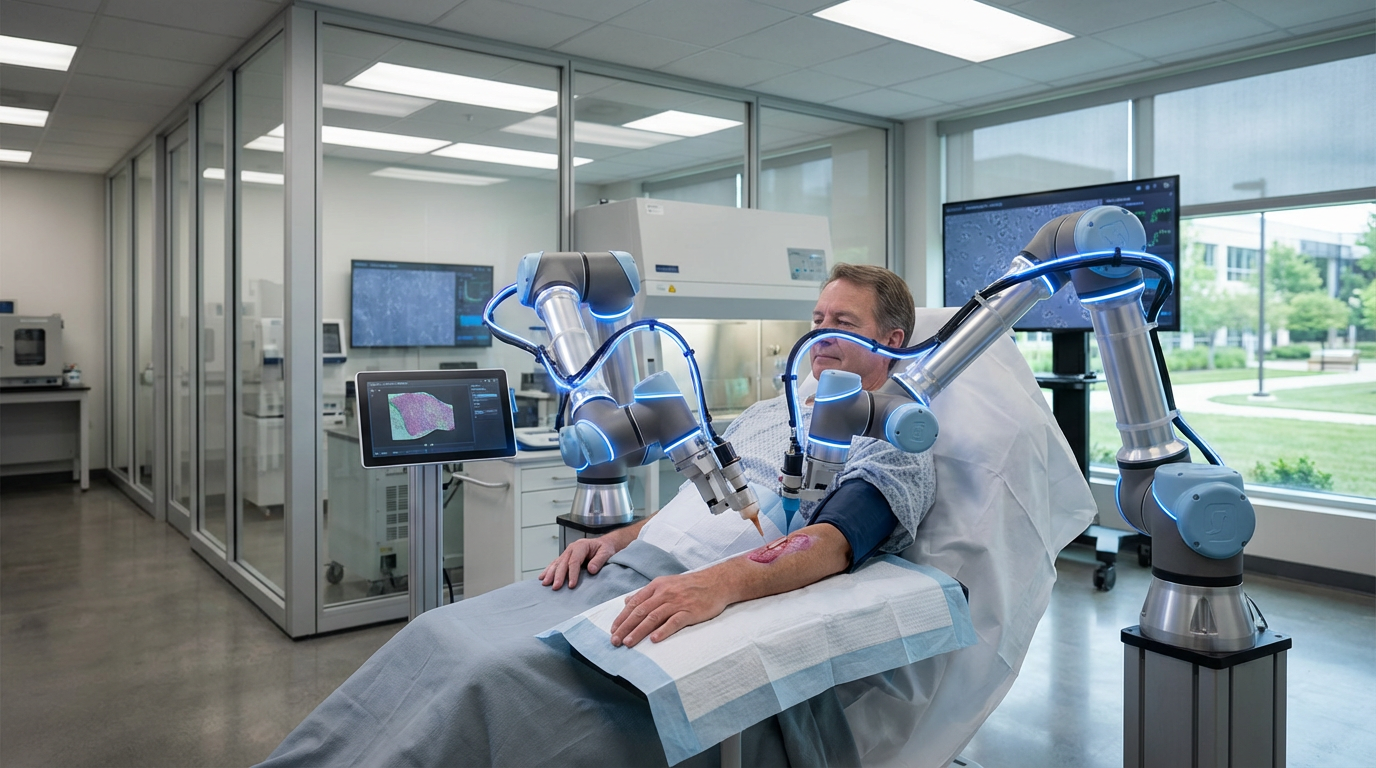
Whole-Organ Regeneration Bioreactors
The shortage of viable organs for transplantation represents one of the most pressing challenges in modern medicine, with thousands of patients dying annually while waiting for suitable donors. Traditional organ transplantation faces multiple constraints: limited donor availability, immune rejection risks, and the irreversible deterioration of organs both before and after harvest. Whole-organ regeneration bioreactors address these fundamental limitations by creating controlled environments where damaged or aged organs can be systematically restored to functional condition outside the human body. These sophisticated systems employ perfusion technology—the continuous circulation of nutrient-rich fluids through an organ's vascular network—to maintain tissue viability while performing complex biological interventions. The process typically begins with decellularization, where chemical and enzymatic treatments strip away the organ's original cells while preserving the extracellular matrix scaffold that provides structural integrity. This scaffold, composed of collagen, elastin, and other proteins, retains the organ's three-dimensional architecture and vascular pathways. Advanced bioreactors then precisely control temperature, pressure, oxygen levels, and biochemical signaling molecules to create optimal conditions for reseeding this scaffold with patient-derived induced pluripotent stem cells that have been differentiated into organ-specific cell types.
The implications for regenerative medicine and transplantation are profound. By enabling the restoration of marginal donor organs previously deemed unsuitable for transplant, these bioreactors could dramatically expand the available organ pool. Research suggests that organs damaged by ischemia, infection, or the donor's age-related decline might be salvaged and rejuvenated through ex vivo treatment cycles lasting days to weeks. This technology also addresses the chronic shortage of pediatric organs by potentially allowing adult organs to be resized and recellularized for younger recipients. Furthermore, the ability to use a patient's own stem cells for recellularization could significantly reduce or eliminate the need for lifelong immunosuppression, which currently carries substantial health risks and costs. Early laboratory demonstrations have shown promise in regenerating functional liver, kidney, and lung tissue, though challenges remain in achieving complete vascularization and restoring the complex cellular diversity found in native organs. The technology also opens possibilities for organ enhancement, where bioreactors might not merely restore function but actively remove senescent cells and repair age-related damage, potentially extending organ lifespan beyond natural limits.
Current development efforts focus primarily on preclinical research, with several academic medical centers and biotechnology companies working to refine perfusion protocols and cell-seeding techniques. While fully regenerated human organs suitable for clinical transplantation remain years away, intermediate applications are emerging more rapidly. Some facilities are already using simpler perfusion systems to preserve and assess donor organs during transport, extending viable storage times and improving transplant outcomes. The technology also serves as a powerful research platform, allowing scientists to study organ development, disease progression, and drug responses in intact human tissue outside the body. As bioengineering capabilities advance and our understanding of stem cell differentiation deepens, whole-organ regeneration bioreactors represent a convergence of multiple cutting-edge fields—tissue engineering, microfluidics, computational biology, and regenerative medicine. This convergence points toward a future where organ failure might be treated not through scarce transplants but through systematic biological restoration, fundamentally transforming the relationship between aging, disease, and organ function in the broader context of human longevity extension.
Related Organizations
A biotechnology company developing bioengineered organs for transplant.
Developer of the Organ Care System (OCS), a portable normothermic perfusion platform for heart, lung, and liver transplantation.
Creators of the metra system, which preserves donor livers at body temperature for up to 24 hours prior to transplant.
Biotech company with a major division dedicated to manufacturing transplantable organs (lungs, kidneys) via bioprinting.

XVIVO Perfusion
Sweden · Company
A medical technology company focused on developing optimized solutions for organ, tissue, and cell preservation.
A premier research institute led by Dr. Anthony Atala, famous for printing bladders and developing the ITOP printer.
A manufacturer of specialized physiological research equipment.
Developed the SWIFT (Sacrificial Writing into Functional Tissue) method for 3D printing vascular channels in living matrices.
Develops a multi-organ-chip platform that simulates the interaction between different organs in the human body.