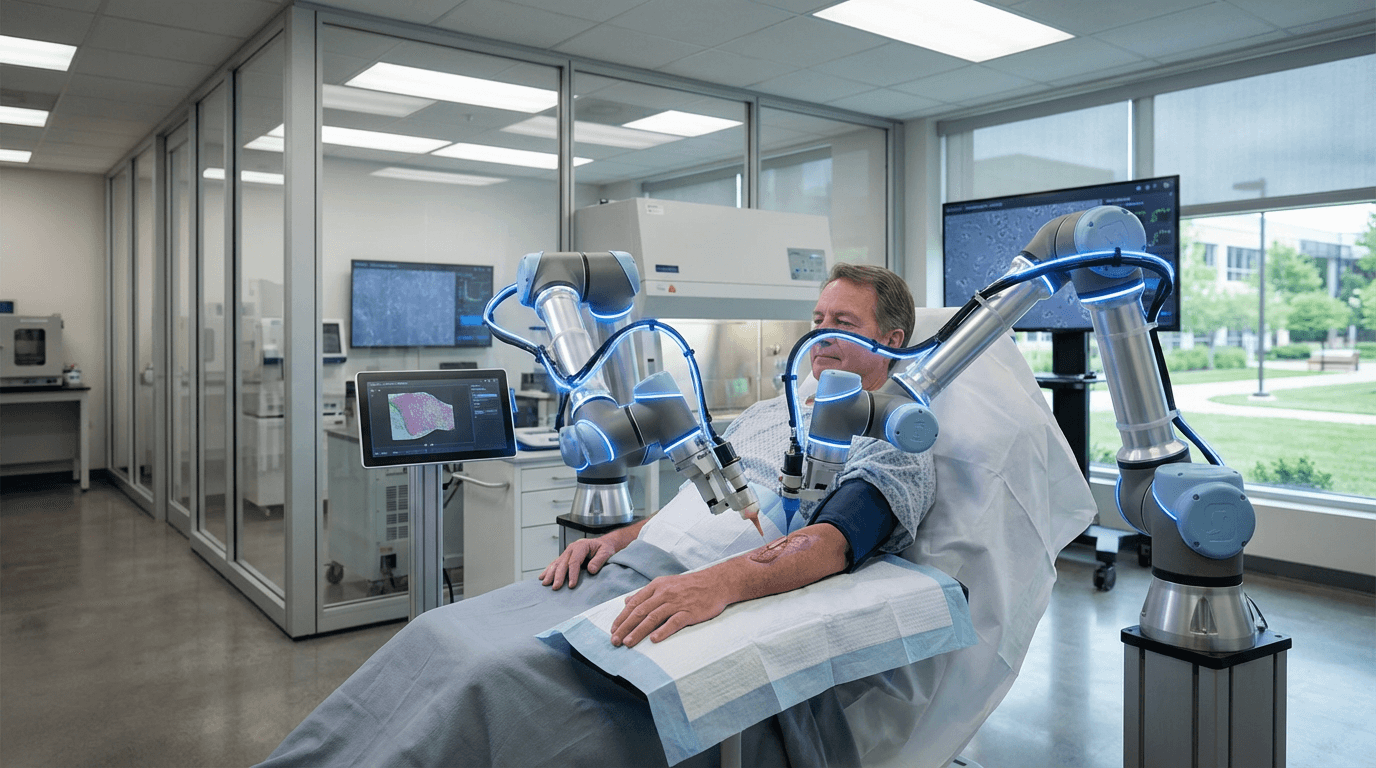
In-Situ Bioprinting Arms
In-situ bioprinting arms represent a convergence of robotics, regenerative medicine, and additive manufacturing, designed to address one of healthcare's most persistent challenges: the rapid and effective treatment of severe tissue damage. These sophisticated robotic systems integrate advanced imaging sensors—typically combining 3D scanning, thermal imaging, and depth perception—with precision bioprinting nozzles capable of depositing living cells and biomaterials directly onto damaged tissue. The technology operates by first mapping the wound geometry in real-time, creating a digital model that guides the robotic arm's movements with sub-millimeter accuracy. The bio-ink cartridges contain carefully formulated combinations of patient-derived or donor cells, growth factors, extracellular matrix proteins, and biodegradable scaffolding materials that provide structural support while promoting natural tissue regeneration. Unlike traditional bioprinting methods that create tissue constructs in laboratory settings, in-situ systems eliminate the need for tissue maturation periods and complex transplantation procedures by building new tissue layer by layer directly where it's needed.
The primary challenge this technology addresses is the limited regenerative capacity of human tissue, particularly in cases of extensive burns, chronic wounds, and traumatic injuries where conventional treatments often result in prolonged healing times, significant scarring, and functional impairment. Traditional wound care relies on skin grafts harvested from other body areas—a painful process that creates secondary wounds—or synthetic dressings that merely protect rather than actively regenerate tissue. In-situ bioprinting fundamentally transforms this paradigm by enabling personalized, on-demand tissue fabrication that matches the patient's specific cellular composition and wound architecture. Research suggests this approach significantly reduces healing times compared to conventional methods, while the precise deposition of growth factors and cells promotes more organized tissue formation, potentially minimizing scar tissue development. For military medicine and emergency trauma care, these systems offer the possibility of treating severe injuries in field hospitals or disaster zones, where access to specialized burn centers or tissue banks may be limited.
Early clinical trials and pilot programs have demonstrated the feasibility of in-situ bioprinting for treating partial-thickness burns and chronic diabetic ulcers, with some systems showing promising results in accelerating wound closure rates. The technology is currently transitioning from research laboratories to controlled clinical environments, though widespread adoption faces challenges including regulatory approval processes, the complexity of maintaining viable cell cultures in clinical settings, and the substantial cost of the robotic systems and bio-ink materials. Industry analysts note growing interest from military medical research programs and major medical device manufacturers in developing portable versions of these systems. As the technology matures, applications may extend beyond wound healing to include in-situ printing of vascular structures during surgery, direct printing of cartilage for joint repair, and even the reconstruction of complex facial tissues following trauma. The convergence of this technology with advances in stem cell biology and personalized medicine suggests a future where tissue regeneration becomes an increasingly routine aspect of surgical and emergency care, fundamentally altering treatment protocols for conditions that currently result in permanent tissue loss or disfigurement.
Related Organizations
A premier research institute led by Dr. Anthony Atala, famous for printing bladders and developing the ITOP printer.
Produces the RASTRUM platform, a drop-on-demand 3D bioprinter for high-throughput cell models.
Develops the Dr. INVIVO 4D bioprinter series for organ regeneration and skin printing.
The academic home of Geoffrey Hinton and a primary feeder for the Vector Institute.
Home to the ARC Centre of Excellence for Electromaterials Science (ACES), focusing on 4D printing.

Poietis
France · Company
Uses laser-assisted bioprinting (LAB) to print living cells with single-cell resolution.
Focuses on 4D bio-fabrication for ophthalmology, printing tissues that can be transplanted or potentially printed in-situ.
Uses microfluidic 3D bioprinting technology to create bioprinted therapeutics, partnering with Novo Nordisk.









