Wireless Neonatal Sensors
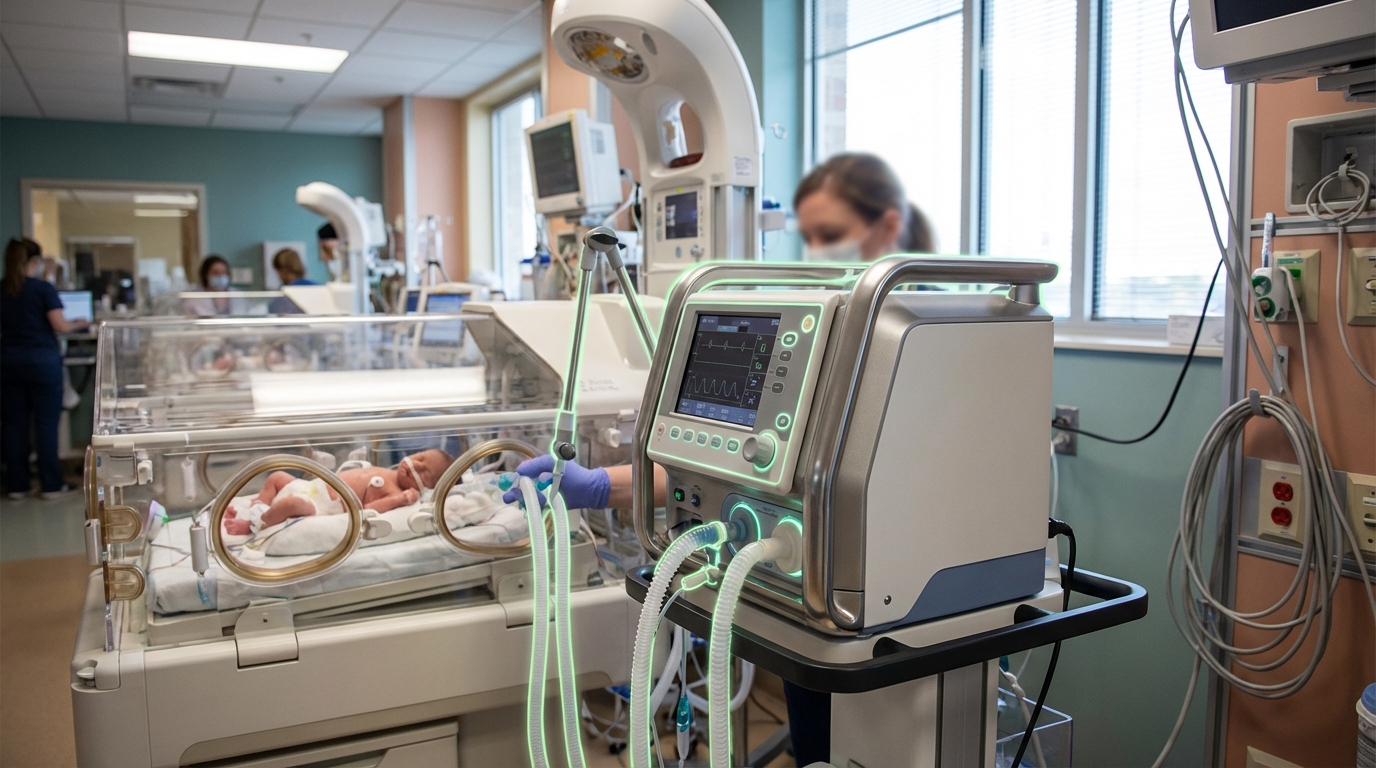
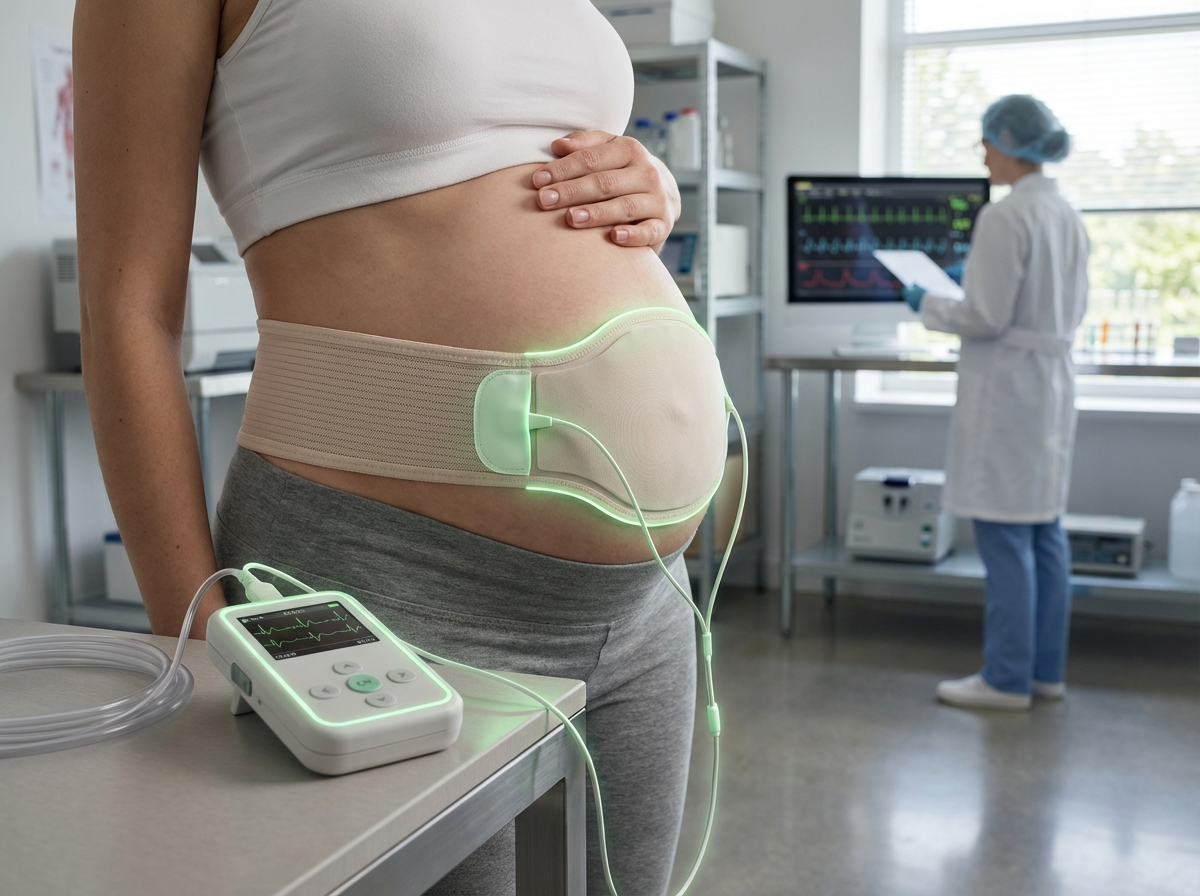
Wireless neonatal sensors represent a significant advancement in neonatal intensive care unit (NICU) technology, addressing the critical need for continuous vital sign monitoring in premature and critically ill newborns. These devices employ soft, skin-like materials—often based on flexible electronics and biocompatible polymers—that conform to the delicate skin of neonates without causing irritation or damage. Unlike traditional monitoring systems that rely on adhesive electrodes, rigid probes, and tangled wires, these sensors use advanced materials science to create ultra-thin, stretchable circuits that can bend and move with an infant's body. The wireless transmission of data, typically through low-power radio frequencies or near-field communication protocols, eliminates the physical tethers that have long characterized NICU care, while integrated sensors continuously track heart rate, respiratory rate, oxygen saturation, temperature, and other critical physiological parameters.
The neonatal care environment has historically faced a fundamental tension between the need for comprehensive monitoring and the risks posed by traditional equipment. Conventional wired sensors create multiple challenges: they restrict movement, complicate parent-infant bonding through skin-to-skin contact, increase the risk of infection through multiple attachment points, and can cause skin breakdown in premature infants whose epidermal layers are not fully developed. The weight and stiffness of traditional monitoring equipment can also interfere with proper positioning of fragile infants, while the maze of wires complicates routine care procedures and increases the likelihood of accidental disconnections that trigger false alarms. Wireless neonatal sensors fundamentally transform this paradigm by enabling what researchers describe as "untethered monitoring," where comprehensive physiological data collection occurs without the physical and clinical burdens of conventional systems. This technology also supports earlier parent-infant interaction, a factor increasingly recognized as crucial for developmental outcomes, while reducing the stress levels associated with NICU environments for both infants and families.
Early clinical deployments of wireless neonatal sensors have demonstrated promising results in reducing skin injuries and facilitating kangaroo care—the practice of holding infants skin-to-skin—which has been shown to improve outcomes in premature babies. Several academic medical centers have incorporated these systems into their NICUs, reporting fewer false alarms, reduced handling stress for infants, and improved workflow efficiency for nursing staff. The technology aligns with broader trends in neonatal care toward gentler, more developmentally appropriate interventions that minimize iatrogenic harm while maintaining rigorous clinical oversight. As sensor miniaturization continues and battery technology improves, future iterations may incorporate additional monitoring capabilities such as continuous blood pressure measurement or biochemical sensing, further expanding the potential for comprehensive yet minimally invasive neonatal care. The convergence of flexible electronics, wireless communication, and evidence-based neonatal practices positions these sensors as a cornerstone technology for next-generation NICUs focused on both clinical excellence and family-centered care.
Related Organizations
Spun out of Northwestern University, developing soft, flexible sensors for ICU-grade monitoring in the home.
Develops the Bambi Belt, a wireless, skin-friendly neonatal vital sign monitoring system designed to replace adhesive electrodes.
Home to the Cognitive Neuroscience Lab (Ken Paller), which pioneered two-way communication with lucid dreamers and memory reactivation during sleep.
Creates neoGuard, a wireless wearable vital signs monitor for newborns in low-resource settings.
One of the largest private foundations in the world.
Develops ultrasound systems (Voluson) with AI features that assist in assessing fetal development and cervical length, key indicators for preterm risk.
Global health technology company with a strong portfolio in patient monitoring and telehealth.
International leader in the fields of medical and safety technology.
Partners to deploy innovative newborn survival technologies, including heart rate monitors, in low-resource settings.