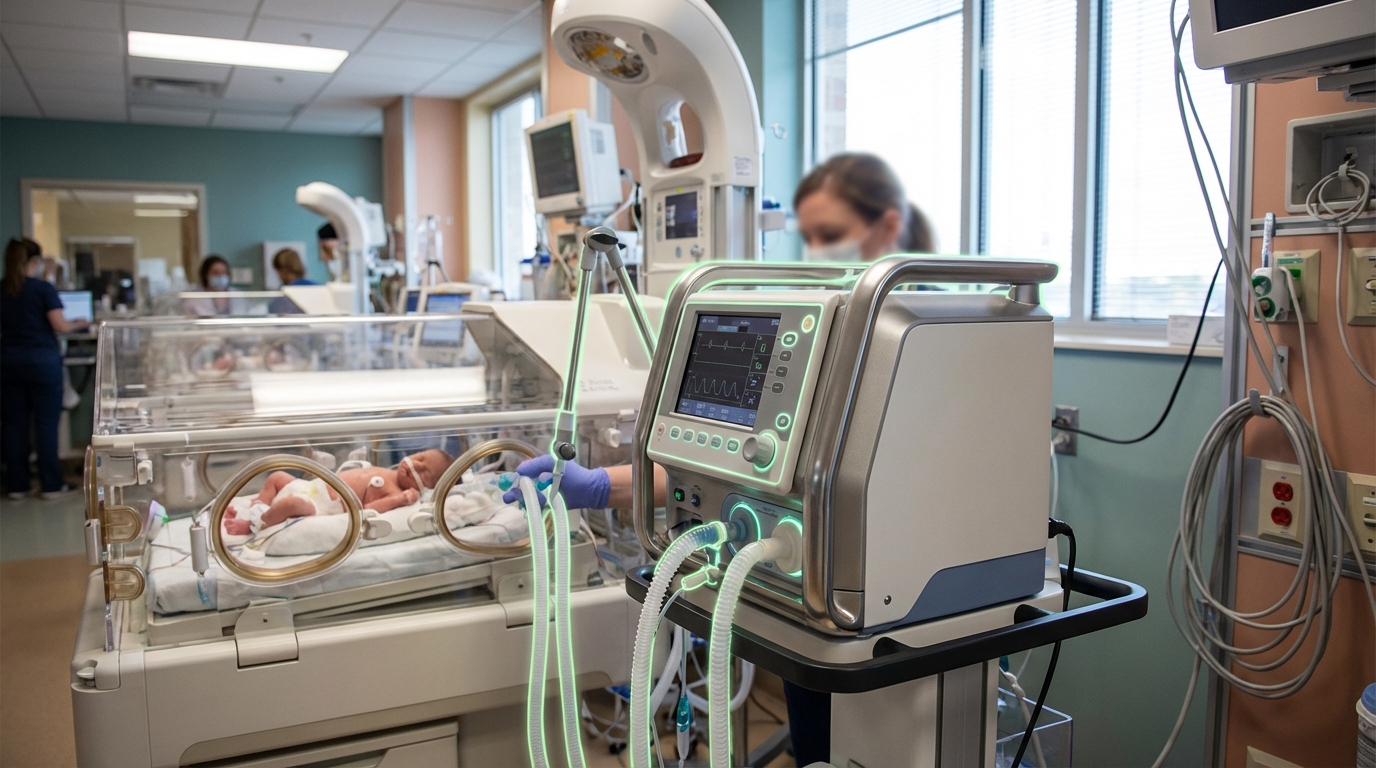
Neonatal Digital Twins
Neonatal digital twins represent a sophisticated computational approach to modeling the complex physiological systems of newborn infants, particularly those requiring intensive care. These virtual replicas integrate real-time patient data—including vital signs, laboratory results, imaging studies, and continuous monitoring metrics—with advanced physiological models to create dynamic, individualized simulations of an infant's biological responses. The technology relies on machine learning algorithms, computational fluid dynamics, and systems biology principles to construct models that can mirror cardiovascular function, respiratory mechanics, metabolic processes, and neurological development. By continuously updating these models with incoming patient data from NICU monitoring equipment, the digital twin evolves alongside the actual infant, creating an increasingly accurate representation that can predict how the baby might respond to various clinical interventions before they are administered.
The neonatal intensive care unit presents unique challenges that make digital twin technology particularly valuable. Premature infants and critically ill newborns have rapidly changing physiology, limited physiological reserves, and heightened vulnerability to adverse drug reactions or treatment complications. Traditional trial-and-error approaches to optimizing ventilator settings, medication dosages, or nutritional support carry significant risks in this fragile population. Digital twins address these challenges by enabling clinicians to test interventions virtually, simulating outcomes across multiple treatment scenarios to identify the optimal approach for each individual patient. This capability is especially crucial for conditions like respiratory distress syndrome, where ventilator settings must be precisely calibrated to support breathing without causing lung injury, or for managing complex cardiac defects where surgical timing and approach can dramatically impact outcomes. The technology also supports earlier detection of complications by identifying subtle deviations from expected physiological patterns that might not be immediately apparent through conventional monitoring.
Research institutions and specialized children's hospitals have begun piloting neonatal digital twin systems, though widespread clinical adoption remains in early stages. Initial implementations have focused on specific organ systems—such as cardiovascular or respiratory models—before expanding to more comprehensive whole-body simulations. Early deployments indicate potential for reducing length of NICU stays, minimizing exposure to unsuccessful treatments, and improving developmental outcomes by enabling more precise, personalized care strategies. As computational power increases and physiological modeling becomes more sophisticated, these systems are expected to integrate genetic information, maternal health data, and environmental factors to provide even more comprehensive predictions. The technology aligns with broader trends toward precision medicine and data-driven healthcare, representing a significant step toward transforming neonatal care from reactive treatment to proactive, simulation-guided intervention that could fundamentally improve survival rates and long-term health outcomes for the most vulnerable patients.
Related Organizations
Software corporation specializing in 3D design and digital mock-ups.
Home to the Artemis Project, a big data analytics platform for neonatal intensive care.
A major pediatric teaching hospital in Toronto.
A major medical technology company offering 'AI-Rad Companion', a family of AI-powered, cloud-based augmented workflow solutions.
An international non-profit organization connecting the VPH community.
Long-standing leader in neuro-symbolic AI, combining neural networks with logical reasoning for enterprise applications.
The largest medical organization in Austria.
Provides patient-specific digital models (Sim&Size) for neurovascular interventions, specifically aneurysm treatment.