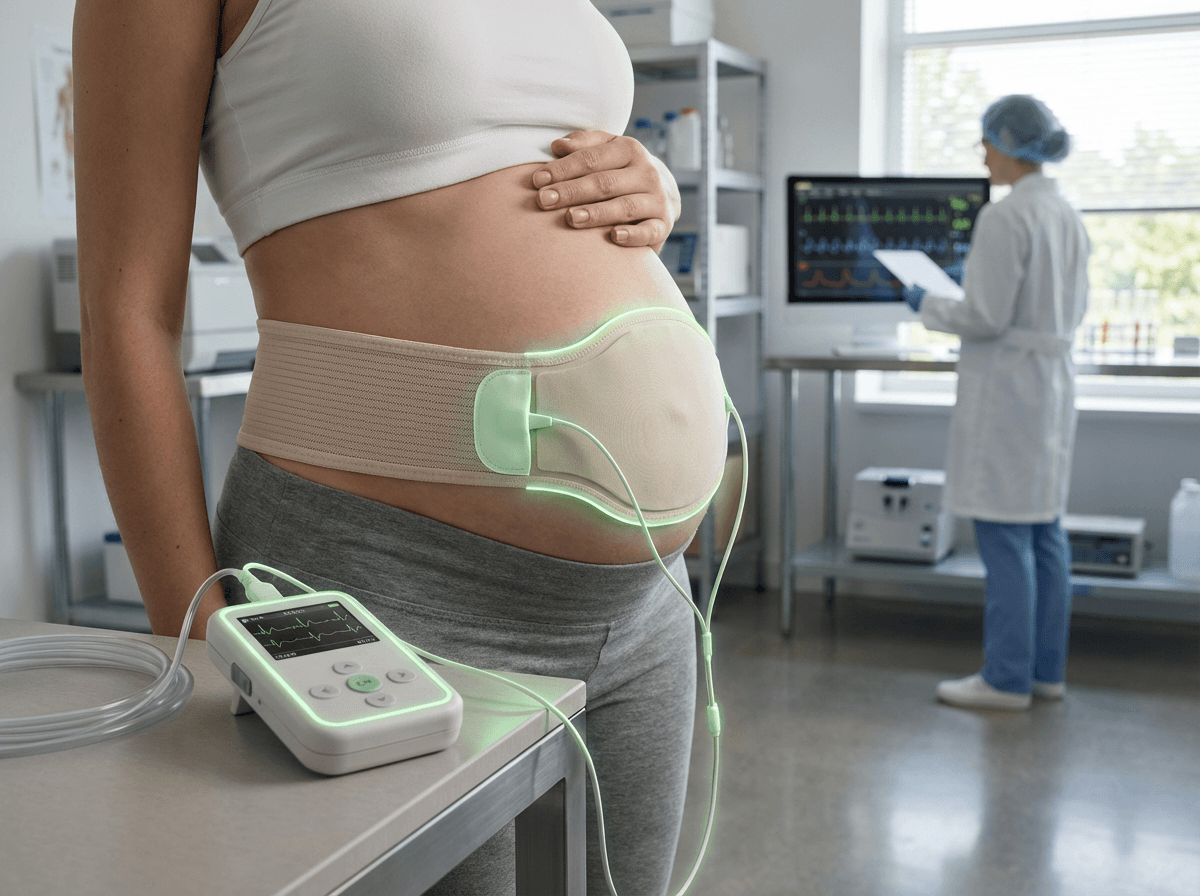
Wearable Uterine Monitoring Patches
Wearable uterine monitoring patches represent a significant advancement in maternal health technology, utilizing thin, flexible sensors that adhere to the abdomen to continuously track uterine activity through electromyography (EMG) and hemodynamic measurements. These patches employ biocompatible electrodes and microfluidic sensors to detect the electrical signals generated by uterine muscle contractions, while simultaneously monitoring blood flow patterns and fetal movements. The technology works by capturing the subtle electrical activity of the myometrium—the muscular layer of the uterus—which changes distinctly as pregnancy progresses and particularly as labor approaches. Unlike traditional tocodynamometry, which requires clinical visits and bulky equipment, these patches use wireless connectivity to transmit data to smartphones or cloud-based platforms, where algorithms analyze patterns that may indicate preterm labor risk, abnormal contractions, or other complications requiring medical attention.
The primary challenge these devices address is the limited ability of current prenatal care models to provide continuous monitoring between clinical appointments, a gap that can result in delayed detection of preterm labor—a leading cause of neonatal mortality and long-term developmental complications. Traditional monitoring methods require pregnant individuals to visit healthcare facilities for intermittent assessments, making it difficult to capture the dynamic changes in uterine activity that occur throughout the day and night. This technology enables early identification of concerning patterns, such as increased contraction frequency or irregular uterine electrical activity, allowing healthcare providers to intervene before complications escalate. For high-risk pregnancies, including those involving multiples, previous preterm births, or certain medical conditions, continuous monitoring can be particularly valuable in reducing unnecessary hospitalizations while ensuring timely intervention when truly needed.
Research institutions and medical device companies have begun piloting these patches in clinical settings, with early deployments focusing on high-risk obstetric populations. Some systems are being evaluated for their ability to predict preterm labor days or weeks in advance by detecting subtle changes in uterine electrical patterns that precede clinical symptoms. The technology also shows promise for managing pregnancies complicated by conditions such as placental insufficiency, where continuous hemodynamic monitoring could provide early warnings of deteriorating fetal blood supply. As the technology matures, industry analysts note its potential to shift prenatal care toward a more proactive, data-driven model, particularly in underserved communities where access to frequent clinical monitoring is limited. The integration of these patches with telemedicine platforms could enable remote pregnancy management, reducing the burden of travel for expectant mothers while maintaining or even improving the quality of surveillance compared to traditional care models.





