Labor Decision Support AI
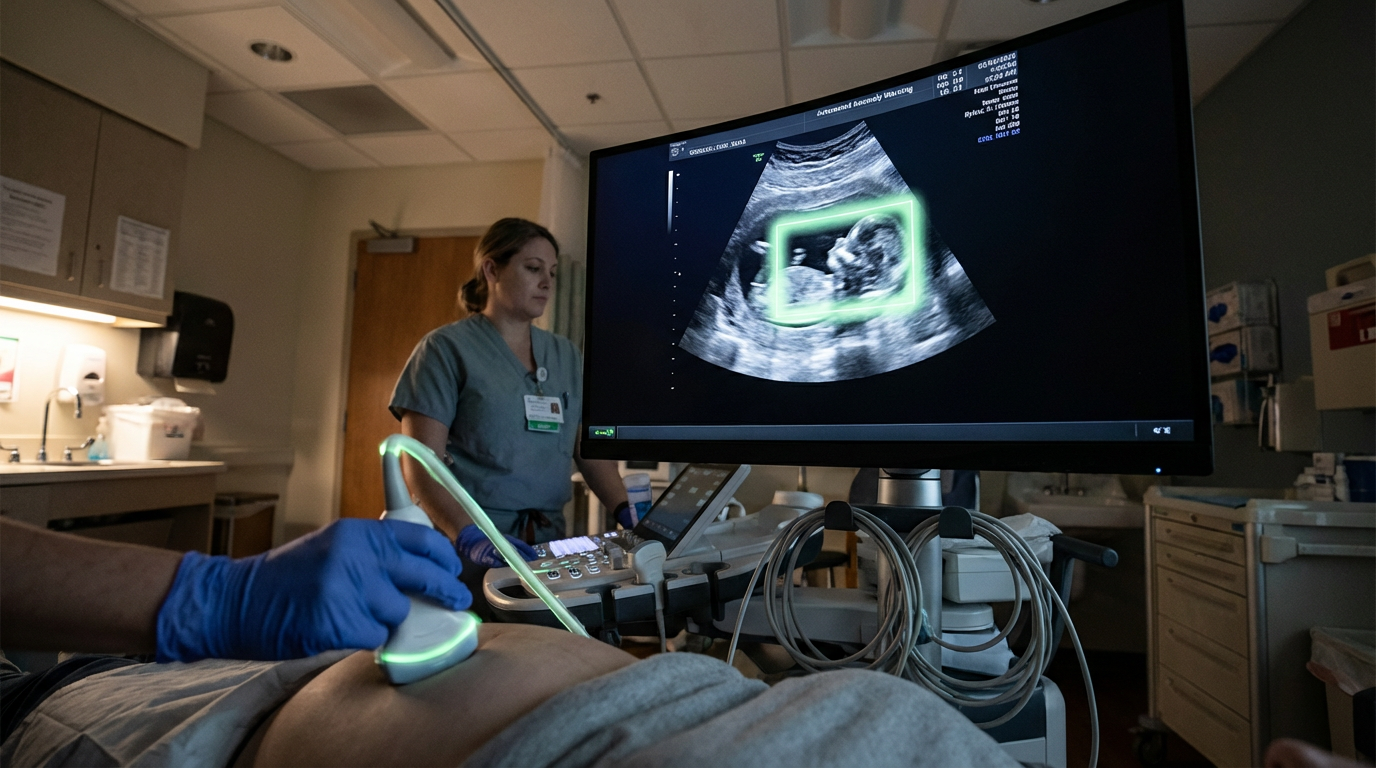
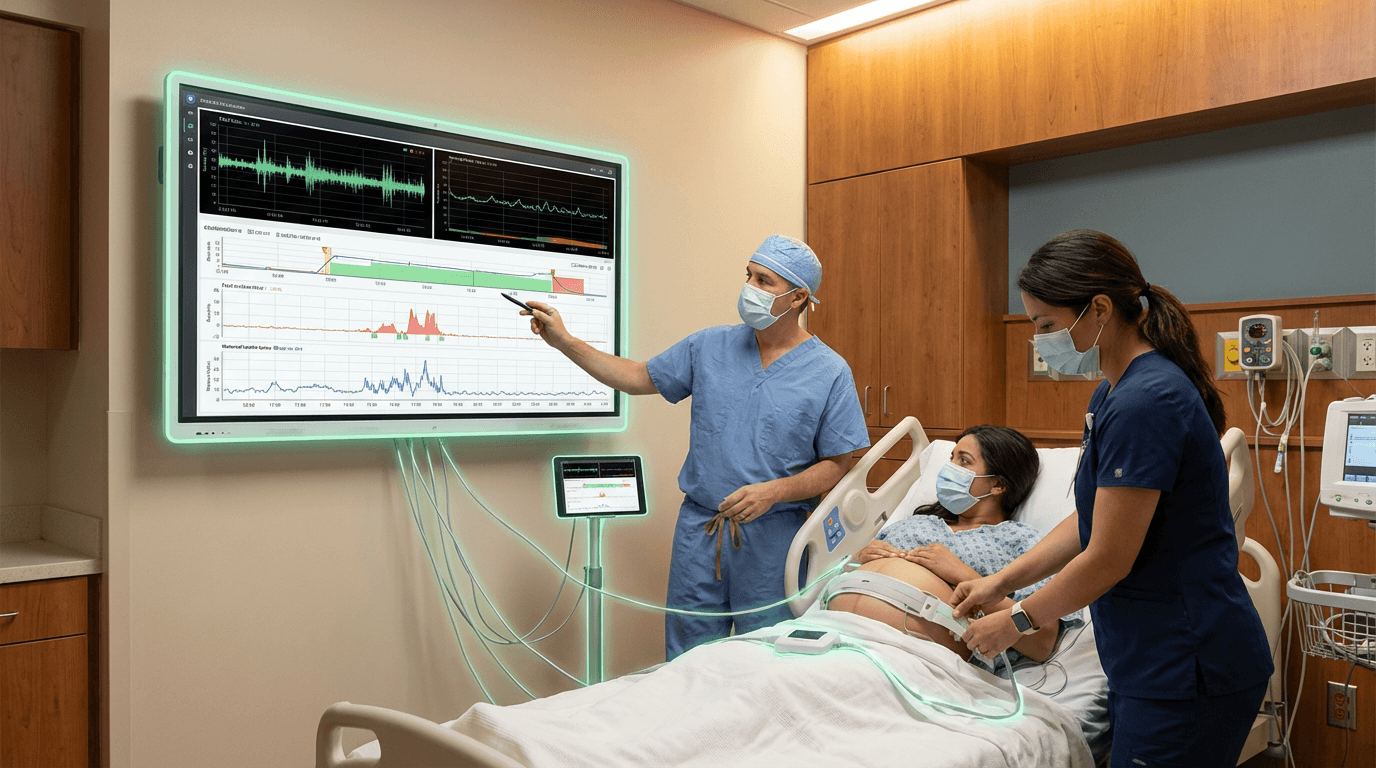
Labor Decision Support AI represents a critical advancement in obstetric care, addressing one of the most challenging aspects of childbirth: the real-time interpretation of complex physiological signals during active labor. At its technical core, these systems employ machine learning algorithms trained on extensive datasets of cardiotocography (CTG) readings, maternal vital signs, contraction patterns, and labor progression metrics. The technology continuously analyzes fetal heart rate variability, baseline patterns, accelerations, and decelerations alongside maternal blood pressure, oxygen saturation, and cervical dilation progress. By processing these multiple data streams simultaneously, the AI identifies subtle patterns and correlations that may escape human observation during the intense, time-pressured environment of labor and delivery. Advanced implementations incorporate deep learning architectures capable of distinguishing between benign variations and genuine indicators of fetal compromise, such as hypoxia or umbilical cord compression, while accounting for individual patient factors including gestational age, maternal health conditions, and labor stage.
The primary challenge these systems address is the inherent difficulty in interpreting CTG traces, which have historically suffered from high inter-observer variability and false-positive rates that can lead to unnecessary cesarean sections. Research suggests that even experienced obstetricians may disagree on CTG interpretation in up to 30 percent of cases, creating uncertainty during critical decision-making moments. Labor Decision Support AI helps standardize this interpretation process, providing consistent, evidence-based risk assessments that support rather than replace clinical judgment. By flagging concerning patterns earlier and with greater specificity, these systems enable care teams to intervene proactively—whether through position changes, oxygen administration, or expedited delivery—potentially reducing both emergency cesarean rates and adverse neonatal outcomes. The technology also addresses staffing challenges in labor and delivery units by extending the monitoring capabilities of available personnel, ensuring that high-risk situations receive immediate attention even when multiple patients are in active labor simultaneously.
Early clinical deployments indicate promising results in reducing decision-making delays and improving communication among multidisciplinary care teams. Several hospital systems have begun piloting these platforms in their labor and delivery units, integrating them with existing electronic health record systems and fetal monitoring equipment. The technology proves particularly valuable in settings with limited access to specialized obstetric expertise, such as rural hospitals or facilities in developing regions, where it can provide decision support comparable to that available at tertiary care centers. As the technology matures, developers are expanding its capabilities to include predictive models for labor duration, likelihood of successful vaginal delivery, and optimal timing for interventions. This evolution aligns with broader trends toward precision medicine in maternal-fetal care, where individualized risk assessment and personalized care pathways promise to improve outcomes for both mothers and newborns. The integration of Labor Decision Support AI into standard obstetric practice represents a significant step toward reducing preventable birth injuries and maternal complications while supporting clinicians in making the most informed decisions possible during one of life's most critical moments.
Related Organizations
Develops PeriWatch Vigilance, an AI-based maternal-fetal early warning system that analyzes fetal heart rate patterns during labor.
Developing a non-invasive fetal oximeter (Lumerah) to better detect fetal distress during labor and reduce unnecessary C-sections.
Develops a wearable patch for tracking contractions and maternal health parameters at home.
Develops ultrasound systems (Voluson) with AI features that assist in assessing fetal development and cervical length, key indicators for preterm risk.
Home to the OxSys research group, which has spent decades developing computerized analysis of fetal heart rate (CTG).
A leading provider of fetal dopplers and monitoring systems used in labor wards globally.
Develops the PreTRM Test, a blood test using proteomic biomarkers and AI to predict the risk of spontaneous preterm birth.