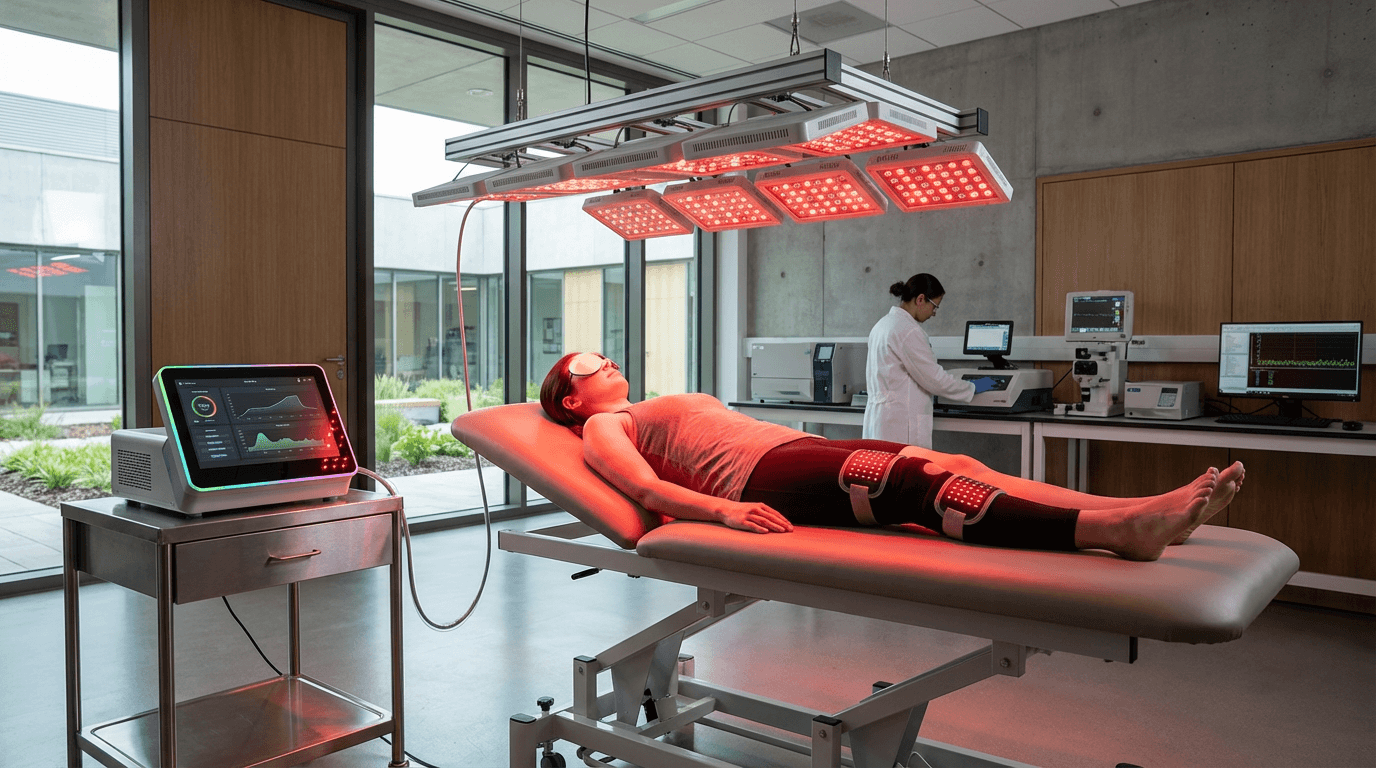
Photobiomodulation Therapy (PBMT)
Photobiomodulation Therapy (PBMT) represents a non-invasive therapeutic approach that harnesses specific wavelengths of red and near-infrared light—typically ranging from 600 to 1000 nanometers—to stimulate biological processes at the cellular level. The fundamental mechanism centers on the absorption of photons by mitochondrial chromophores, particularly cytochrome c oxidase, an enzyme critical to cellular energy production. When these light-sensitive molecules absorb photons within the therapeutic window, they trigger a cascade of cellular responses including enhanced adenosine triphosphate (ATP) synthesis, modulation of reactive oxygen species, and activation of transcription factors that influence cell proliferation and survival. Unlike thermal or ablative laser therapies, PBMT operates at low power densities that produce photochemical rather than thermal effects, making it suitable for treating surface tissues and shallow structures without causing damage. The therapy's effectiveness depends critically on precise dosimetry—the combination of wavelength, power density, treatment duration, and total energy delivered—which must be carefully calibrated to the target tissue depth and therapeutic objective.
The clinical appeal of PBMT lies in its ability to address persistent challenges in pain management, tissue repair, and inflammation control without the side effects associated with pharmaceutical interventions or invasive procedures. Chronic pain conditions, sports injuries, wound healing complications, and inflammatory disorders represent substantial healthcare burdens where conventional treatments often prove inadequate or carry significant risks. PBMT offers a complementary or alternative pathway by accelerating natural healing processes, reducing inflammation through modulation of pro-inflammatory cytokines, and providing analgesic effects through nerve desensitisation and endorphin release. This positions the technology as particularly valuable in rehabilitation medicine, sports medicine, and dermatology, where recovery time and treatment tolerability directly impact patient outcomes and quality of life. The growing body of clinical evidence supporting PBMT's efficacy has driven demand for standardised treatment protocols and medical-grade devices that can deliver consistent, reproducible doses—a shift that distinguishes therapeutic applications from the broader consumer wellness market where claims often outpace scientific validation.
Current adoption of PBMT spans clinical settings ranging from physical therapy practices and sports medicine facilities to dental offices and dermatology clinics, with devices varying from handheld units for localised treatment to full-body panels for systemic applications. Research institutions continue to explore optimal parameters for specific conditions, investigating how factors such as pulsed versus continuous wave delivery, treatment frequency, and patient-specific variables influence outcomes. The technology's integration into mainstream healthcare faces ongoing challenges around treatment standardisation, insurance reimbursement, and the need for larger-scale clinical trials to establish definitive protocols. However, the convergence of improved LED technology, sophisticated dosimetry controls, and real-time monitoring capabilities is advancing PBMT toward more precise, personalised therapeutic applications. As the lighting industry develops increasingly efficient and targeted light sources, and as clinical research refines our understanding of photobiomodulation mechanisms, this therapy is positioned to expand beyond current applications into areas such as neuroprotection, metabolic disorders, and preventive medicine, representing a growing intersection between photonics engineering and evidence-based healthcare.

